Introduction
Frostbite occurs when skin and other tissues are exposed to very cold temperatures. It can happen within minutes following exposure to extreme temperatures, or even in above freezing temperatures if there is a strong wind (wind chill), or if the person is wet or at a high altitude. Frostbite usually affects the hands, feet, nose, cheeks, and ears. Superficial frostbite injures the skin and tissues just beneath the skin, but usually does not permanently injure tissue. Deep frostbite, which also affects muscle, nerves, and blood vessels, may result in tissue death, a condition known as gangrene.
Signs and Symptoms
The following are signs and symptoms of frostbite:
- Pain or prickling progressing to numbness
- Pale, hard, and cold skin with waxy appearance
- Flushing from blood rushing to area after it’s rewarmed
- Burning sensation and swelling from collected fluid that may last for weeks
- Blisters
- Black scab like crust, which may develop several weeks after exposure
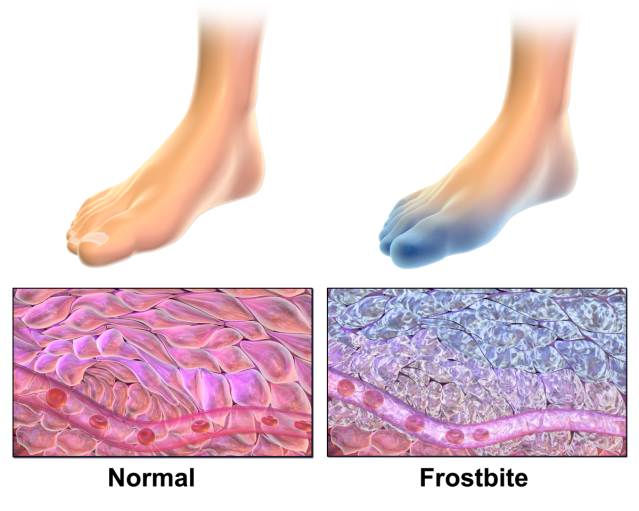
What Causes It?
When exposed to cold, the body tries to preserve heat. Blood vessels near the skin’s surface narrow, forcing more blood into the core to keep the heart and lungs warm. This helps prevent hypothermia, which results when the body’s temperature falls below 98 °F (34 °C). However, it also prevents the extremities (such as hands and feet) from receiving enough blood, which causes them to become cold. At first, the blood vessels alternate between narrowing and widening, to keep the extremities as warm as possible. But under extremely cold conditions, the vessels stop widening. When skin temperature drops low enough, ice crystals can form around and within the cells, freezing tissue and possibly rupturing cells. The lack of circulation that occurs when the body directs blood flow away from the extremities may also cause cell damage.
Who’s Most At Risk?
These factors increase the risk for frostbite:
- Intoxication with alcohol or other substances
- Very young or very old age
- Cardiovascular disease
- Peripheral vascular disease (narrowing of blood vessels in the extremities)
- Poor circulation
- Taking beta-blockers
- Diabetes
- Hypothyroidism
- Exhaustion, hunger, malnutrition, or dehydration
- Winter sports, especially at high altitudes
- Outdoor work
- Windy and or wet weather
- Homelessness
- Severe injury
- Smoking
- Depression
- Previous frostbite
- Skin damage
- Constricting clothing and footwear
What to Expect at Your Provider’s Office
Seek emergency medical care to treat frostbite as soon as possible. Your health care provider will ask about your exposure to cold, including what the temperature was and length of exposure. Your health care provider will also examine your skin, looking for signs of superficial and deep injury. You may not be able to see the extent of your injury until the area rewarms. Doctors may run blood tests and imaging studies, such as magnetic resonance imaging (MRI), to determine the severity of your injury, as well as any complications, such as infection.
Treatment Options
Prevention
If you are going to be outside in cold temperatures, it’s essential to prevent frostbite. Take these steps to keep warm:
- Wear several layers of warm clothing that allow you to move while providing protection from wind and water.
- Wear dry, warm gloves, socks, and insulated boots. Hands and feet account for 90 percent of injuries.
- Replace wet clothes immediately.
- Cover your head, preferably with earflaps, in extreme conditions. About 30% of heat loss occurs through the head.
- Drink plenty of fluids and eat plenty of food during lengthy outings. Do not drink alcohol, smoke cigarettes, or drink caffeine.
- Watch for the development of white patches on the face and ears of your companions. These may signal frostbite.
Treatment Plan
Frostbite is a medical emergency. It is important to get conventional medical care as soon as possible. Remove constricting or wet clothing and immobilize and insulate the affected areas. Your health care provider will treat mild frostbite by rewarming the affected area, washing it with an antiseptic, and applying a sterile dressing. If medical care is not available immediately, seek shelter and rewarm a mildly frostbitten area by immersing it in warm water (101 to 104° F or 38.3 to 40° C), or by repeatedly applying warm cloths to the area for 30 minutes. Never use hot water, fire, a heating pad, or other dry heat because these methods may burn the skin before the feeling returns. Remove any jewelry from the affected area before rewarming because the area may swell. Never rub or massage frozen body parts, and avoid walking on a frostbitten foot, if possible (however, if you are far from help, it is better to walk on frozen feet than to thaw them out). Wrap the area in dry dressings, putting dressings between fingers and toes to keep them separated. If there is any danger of refreezing, it is best not to thaw the area until you reach warm shelter. Thawing and refreezing can seriously damage tissue.
If there is no danger of refreezing, treat deep frostbite by rapid thawing in a warm water bath. The patient should be hospitalized and have a health care provider elevate the frostbitten area. Medication can help control pain. Health care providers will take steps to prevent or treat any infection. Deep frostbite is often accompanied by hypothermia, a medical emergency that requires hospital care.
Drug Therapies
Your health care provider may prescribe drugs, such as narcotic analgesics to treat pain, nonsteroidal anti-inflammatory drugs (NSAIDs) to treat pain and inflammation, antibiotics to prevent or treat infection, or a tetanus shot to prevent tetanus. Aspirin and ibuprofen may be helpful, but evidence is limited.
Surgical Procedures
If frostbite has caused tissue death in any area, such as a hand or foot, amputation may be necessary. Usually this decision is not made for several months, when the extent of the damage is more evident. (At first, frostbite may look worse than it is because the skin may be more seriously affected than the underlying tissues.) If, however, the person has serious infection, wet gangrene, or pain that won’t respond to treatment, surgery may be required sooner. Studies show that removing dead tissue using new techniques improves the result of surgical treatment, reducing blood loss and enhancing the healing process.
Complementary and Alternative Therapies
It is important to seek conventional care for frostbite as soon as possible to prevent tissue damage. While nutritional supplements may enhance conventional treatment, maintaining the body’s core temperature by dressing warmly, drinking fluids, and eating plenty of food before and during exposure to cold are critical to preventing and treating frostbite.
Nutrition and Supplements
- Vitamin C — One well-designed animal study suggested that vitamin C may have some beneficial effect on frostbite when combined with standard medical treatment.
- Antioxidants — When taken prior to cold exposure, antioxidants may help protect against development of frostbite or other cold related injuries.
Herbs
You may use herbs along with conventional medical treatment for frostbite under the supervision of a qualified practitioner, but you should never use herbs to self-treat the condition. Speak to your physician before using any herbal therapies to make sure they are right for you, and that they do not interfere with conventional treatment.
- Cayenne pepper (Capsicum spp.) in topical form has been used traditionally in China and Japan to treat frostbite.
- Poplar buds (Populus spp. including P. nigra, P. canadensis, and P.tacamahaca), also known as balm of Gilead and balm of Mecca, may be used in mild cases of frostbite as an ointment or other topical formula (containing 20 to 30% bud exudate) to alleviate the pain and reduce the risk of infection associated with frostbite.
- Also used topically are calendula (Calendula officinalis), chamomile (Matricaria recutita), and horsetail (Equisetum arvense).
- Aloe vera in topical form every 6 hours may help prevent further tissue damage.
Homeopathy
Few studies have examined the effectiveness of specific homeopathic remedies. A professional homeopath, however, may recommend one or more of the following treatments for frostbite based on his or her knowledge and clinical experience. Before prescribing a remedy, homeopaths take into account a person’s constitutional type — your physical, emotional, and intellectual makeup. An experienced homeopath assesses all of these factors when determining the most appropriate remedy for a particular individual.
- Agaricus — primary remedy for the burning, itching, redness, and swelling associated with frostbite.
- Apismellifica — for the burning or stinging sensation and redness associated with frostbite, particularly if there is excessive swelling. People who benefit from this remedy may also have a dull pain in the back of the head.
- Carbo vegetabilis — for people who feel faint or who have difficulty breathing.
- Lachesis — for frostbite with a blue or purple discoloration. The skin may bleed easily, and irreversible tissue damage may result if it is not treated. This remedy is most appropriate for people who are restless and unsettled.
- Silicea — for frostbite in thin, frail people who typically feel cold and tired. This remedy is most appropriate for those who have pus-filled wounds.
Massage
Frostbitten areas should never be massaged or vigorously rubbed.
Prognosis/Possible Complications
The outlook for frostbite depends on the depth of tissue injury and can range from complete recovery to amputation.
Possible complications of frostbite include the following:
- Increased sensitivity to cold
- Changed skin color
- Faulty nail growth in an affected hand or foot
- Profuse sweating
- Pain with use of the affected area
- Altered sensation in the affected area
- Arthritis
- Skin cancer
A majority of patients have long-term, residual symptoms including pain, loss of sensation, swelling, hair or nail deformities, and rarely, arthritis.
Following Up
Damage caused by frostbite is not always immediately evident. Health care providers will monitor your condition over weeks or months to determine the severity of your injury. Many patients have long-term symptoms, including pain, numbness, swelling, and hair or nail deformities.
(Information for this article was provided by the University of Maryland Medical Center)
Categories: Apocalypse healthcare

